The science behind BIOFLEX
Compared to traditional treatment, patients recover from
musculoskeletal and peripheral nerve injuries with less scar tissue,
accelerated cell regeneration, and improved function.
Low level laser therapy (now known as photobiomodulation therapy or PBMT) has evolved exponentially since its’ serendipitous discovery in the 1960s by Hungarian physician, Endre Mester.
He went on to design further experiments using this low powered red laser on skin flap wounds and burns in rats as well as diabetic ulcers and infected wounds in humans. Mester observed accelerated healing when exposed to low doses of red laser light.
Mester was attempting to use a high-powered ruby crystal red laser to destroy surgically implanted tumor cells in rats. His laser was mistakenly calibrated to a lower, non-ablative power output, and he observed no tumour changes but noticed faster incision healing and quicker hair regrowth than controls.
He described this phenomenon as “biostimulation.” His research continued into the 1980s using low doses of red light, where he observed increased fibroblast activation, collagen production, anti-inflammatory and analgesic effects, phagocytosis, and systemic immunological responses.
Laser Therapy interacts with photoreceptors to produce photochemical reactions that have a positive effect on cellular metabolism and recovery from damage and inflammation.
BIOFLEX® is the only laser therapy company that utilizes powerful Class 3b lasers together
with large surface arrays of bicolour LEDs that affect a large volume of circulating blood as well as underlying tissues resulting in both a powerful systemic and direct photobiomodulation effect. The overall clinical effect of targeting both the injured/diseased tissues as well as the surrounding circulatory system is an unsurpassed accelerated healing response and decrease in pain, inflammation, edema and associated symptoms.
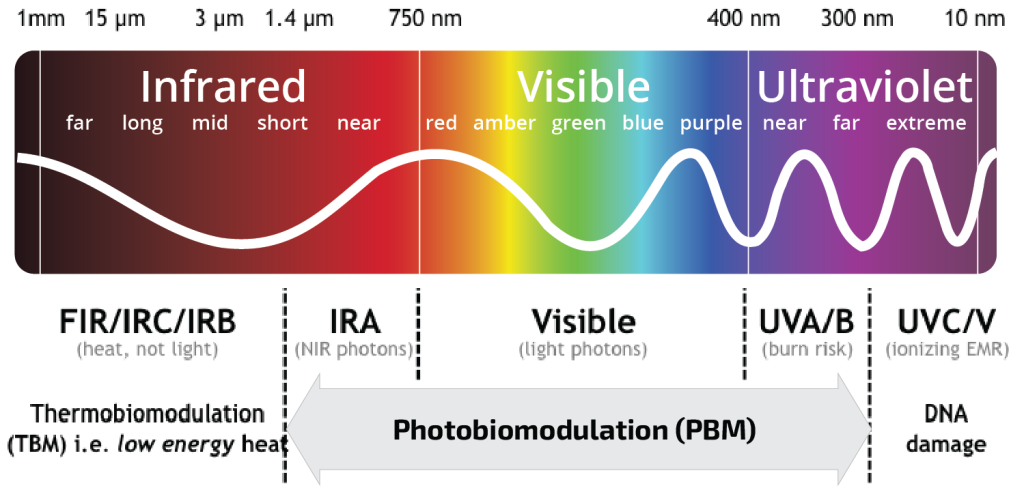
The effectiveness of wavelengths of light with respect to photobiomodulation therapy can be characterized by the action
spectra of the target photoacceptors (e.g. cytochrome c oxidase), that determine the positive biological responses such as
increased metabolism, cellular regeneration and immunomodulation. The most clinically effective wavelength ranges are in
the red (680-630 nm) and near infrared spectra (840-810 nm). Wavelength is one critical parameter of light among other
factors such as dosage or energy density (J/cm2), treatment time and light delivery in pulses (cycles per second or Hz) in
determining the efficiency of absorption, depth of penetration and ultimately the clinical outcomes. The effects of
photobiomodulation are cumulative and can be clinically evident immediately after treatment or over a period of days.
Mechanisms of action

Laser Therapy initially used red wavelengths because ruby red crystal was the only laser medium available. As lasers were developed, different wavelengths were used in research and eventually the mechanisms of action as well as optimal wavelengths were determined.
Mester’s early positive clinical results led to intense scientific research into the cellular and physiological mechanisms of action of laser biostimulation. In the 1980s, Prof. Tiina Karu, a Biophysicist from Moscow was the first scientist to establish the fundamental cellular mechanism of action based on the active absorption spectrum of cytochrome c oxidase (CCO) by red and near infrared wavelengths.
CCO is one of the terminal enzymes of the electron transport chain and is responsible for mitochondrial ATP production. The action spectra in the visible-to-near infrared (NIR) region measured for biological responses showed that the most effective wavelengths for stimulating CCO were in the far-red range (660 and 683.7 nm) and in the NIR bands of 812.5-846.0 nm.
She was able to demonstrate these very specific wavelengths in the red and near infrared spectrum were optimal for activating CCO by disassociating nitric oxide and increasing cellular ATP leading to a cascade of positive cellular effects. A plethora of research into the mechanisms of action has elucidated numerous other beneficial effects including decreased inflammation, cytoprotection, cellular proliferation and migration, increase stem cell activity and protein synthesis.
Establishing the Foundations of Photobiomodulation Therapy
It became evident that the physiological benefits of laser therapy were not limited to laser diodes. In the 1980s, NASA scientists experimenting with red and blue LEDs for plant growth in space observed faster healing of hand abrasions and cuts.
Further research using various light sources—including LEDs, broadband light, and laser diodes—concluded that clinical efficacy depended on light parameters rather than the source itself. This led to the evolution from Low Level Laser Therapy to Low Level Laser/Light Therapy, now known as Photobiomodulation Therapy (PBMT).

PBMT is defined as a form of light therapy that utilizes non-ionizing forms of light sources, including LASERS, LEDs, and broad-band light, in the visible and infrared spectrum. It is a non-thermal process involving endogenous chromophores eliciting photophysical and photochemical events at various biological scales. This process results in beneficial therapeutic outcomes including but not limited to the alleviation of pain or inflammation, immunomodulation, and promotion of wound healing and tissue regeneration.
Eventually the most important PBMT parameters were established and included not only the wavelengths emitted, but also the dose of photons measured in Joules or Joules/cm2 (energy density) imparted directly to the skin at each contact point, treatment time (seconds to minutes) and pulsing parameters (Hz). An explosion of research has resulted in a more concise understanding of the mechanisms of action, depth of penetration as well as establishing a range of effective light doses for different clinical indications.
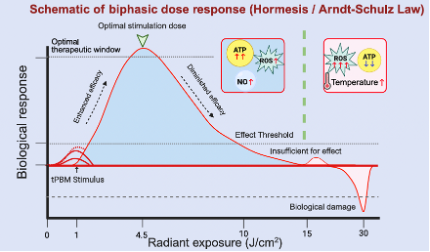
It became clear that there is a biphasic dose response such that positive clinical findings only occur in a “window of light energy”. Too little light energy or dose is not effective, and too much is equally not effective. To achieve optimal clinical outcomes, a clinician needs to understand all these parameters, the diagnosis including depth and affected tissue types. Only then will there be excellent clinical outcomes – an expertise BIOFLEX has refined through 35+ years of research and development.
The Importance Of Red Combined With Near Infrared Light
Infrared light
Near Infrared wavelengths are also known to be absorbed by
cytochrome c oxidase and other photoreceptors that result in
positive effects on cellular physiology. Tiina Karu was the one of the key researchers to establish the photoabsorption spectra of these photoacceptors as well as the ranges of wavelengths that result in optimal photobiomodulation. She observed near infrared wavelengths in the ranges of 800-840 nm were most active, making them more effective for deeper lying injuries and conditions associated with musculoskeletal conditions.
These near infrared wavelengths are much less absorbed by
hemoglobin and other photoacceptors that prevent light from
penetrating more deeply. As a result, light in the range of
800-840 nm are considered to be the most transparent of the
wavelengths used in photobiomodulation therapy allowing for
much deeper effective penetration of several cm. The actual
clinical effective depth of penetration varies as a result of factors like skin colour, tissue density, power, treatment time and using contact technique. Claims of deeper penetration with more power or longer wavelengths are not accurate not supported by the research.
Tissues like bone, tendon, muscle, adipose and ligament vary
with respect how much light can effectively penetrate and
accumulate to a dosage high enough to result in a photobiomodulation effect. When trying to elicit a direct
photobiomodulation effect on these types of tissues, near
infrared wavelengths are the most effective and are the “go to” wavelength range to heal these deeper tissues.
Using greater power is one way to increase the dosage more
quickly in these deeper tissues. However, as power increases
so does the potential for an inhibiting thermal effect. Of course
higher power also means shorter treatment times which results in fewer target photoacceptors being stimulated.
Research has shown longer illumination times result in a greater therapeutic effect. The consensus on how to achieve an optimal photobiomodulation healing effect in deeper tissues is a balance of high enough power with longer treatment times.
Red light
Since the introduction of the He-Ne laser (632.8 nm) in the 1960s, the positive effects of red light wavelengths (λ = 630-680 nm) have been established both in vitro and human clinical trials. These wavelengths are highly absorbed by cytochrome c oxidase, one of the terminal enzymes in the electron transport chain responsible for the creation of ATP. Cells and tissues under metabolic stress due to injury or disease will repair and recover much faster when exposed to these red wavelengths as a direct result of increased ATP production and increased cellular metabolism.
Red wavelengths are also absorbed to some degree by other photoacceptors in the skin including hemoglobin and melanin which limits the effective depth of penetration to the subcutaneous regions of the body (approximately 5-10 mm). Other wavelengths like violet and blue are so highly absorbed by skin photoacceptors that they barely penetrate the skin (1-2 mm) and thus are not used in Laser Therapy with the exception of treating superficial skin conditions like acne.
Red wavelengths principally in the 630-680 nm range are very beneficial for treating conditions that are relatively superficial such as subcutaneous bursitis, skin conditions like acne, psoriasis, hair loss and eczema as well as wounds and chronic ulcers. The large network of capillaries located in the subcutaneous region will also absorb red wavelengths resulting in a powerful immunomodulating effect by the activated white blood cells, stem cells and platelets. This is called a systemic or remote effect and it produces an anti-inflammatory and healing effect that is circulated by the activated white blood cells to injured and diseased tissues deep to the treated area. Even though red light does not penetrate deeply, it can still be a very powerful healing wavelength for deeper tissues provided the dosage of light is adequate. The more blood that is stimulated the stronger the systemic effect of photobiomodulation.
Laser Therapeutic Platforms
The therapeutic effects of Laser Therapy at the cellular level have proven to increase ATP levels and DNA synthesis and are
specific to enhance mitochondrial membrane potential and function. The light emitted using the various laser therapy systems
stimulate the photochemical reactions within the cells supporting mitochondrial activities. This can create beneficial changes
in cell behavior and accelerate the natural healing process. Mitochondria contain photoreceptors that absorb the photons from
light and convert these into ATP – energy that can be utilized to stimulate cellular activities and biological processes. Proper
mitochondrial function and ATP production are critical to the process of neuro-protection modulation, regeneration, cognitive
enhancement, and the prevention and alleviation of a number of other neurological pathologies. Laser Therapy is effective in:

Musculoskeletal Injuries
The most common applications are muscle strains, ligament sprains, tendinopathies, cartilage tears, bursitis and other injuries to the musculoskeletal system. Whether it’s a sports injury, overuse condition, or an accident, the goal of treatment is to accelerate the healing process and decrease symptoms which allows the clinician to initiate manual and exercise therapies much sooner.

Wound Healing
Laser Therapy has been proven to accelerate surgical wound healing, dermal ulcers, diabetic lesions and all other recalcitrant wounds. The effects include increased angiogenesis, neovascularization, collagen secretion and decreased
inflammatory exudate and provides epithelization of the wound, improved arterial perfusion and regeneration of the local and regional tissues.

Arthritis
Chronic progressive forms of joint degeneration can be effectively managed with Laser Therapy. All of the arthritides from early to late stages will respond to treatment resulting in decreased pain, inflammation, stiffness and edema. Research has even shown repair and regeneration of eroded hyaline
cartilage when exposed to Laser Therapy.

Nerve Healing
From diabetic neuropathy to
discogenic radiculopathy to carpal tunnel syndrome, Laser Therapy can accelerate nerve healing and decrease paraesthesia and nerve
pain as a result of direct absorption of light. Many peer reviewed clinical trials and lab studies have proven Laser Therapy is an effective therapy for nerve healing and has no known side effects.